Definitions
- Sliding hiatus hernias are the most common type of hiatus hernias
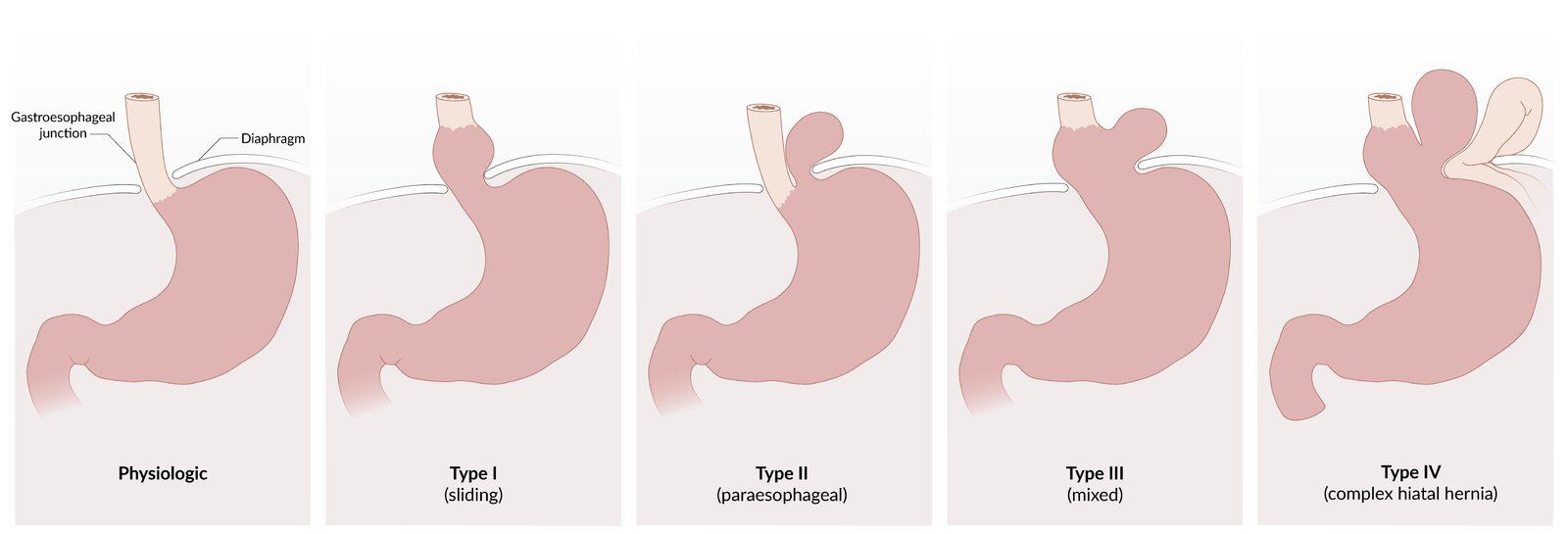
- A type I hiatal hernia is a sliding hiatal hernia
- A type II hiatal hernia is a paraoesophageal hiatal hernia
- A type III hiatal hernia is a mixed hiatal hernia
- A type IV hiatal hernia is a complex hiatal hernia
Risk Factors
- Age → phrenooesophageal ligament weakens
- Obesity → deposition of fat in and around the crura → widened hiatus
- Smoking → loss of elastin fibres in the diaphragmatic crura
- Prolonged periods of increased intra-abdominal pressure for example from:
- Pregnancy
- Ascites
- Chronic cough
- Chronic constipation
Clinical Features
- Most hiatal hernias are asymptomatic and require no medical or surgica intervention
- Type 1 hiatus hernia patients have symptoms similar to Gastroesophageal Reflux Disease (GORD)
- The saint triad is a common triad of pathologies consisting of cholelithiasis, diverticulosis, and hiatal hernia
Investigations and diagnosis
- Barium swallow
- Endoscopy
- Often incidentally found on chest X-ray
Management
- Non-pharmacological
- Pharmacological
- Surgery
- Laparoscopic/open fundoplication and hiatoplasty
- Indicated when:
- Persistence of symptoms despite conservative management
- Refusal or inability to take long-term PPIs
- Severe symptoms/complications of gastroesophageal reflux disease: bleeding, strictures, ulcerations
Complications
- Type I has similar complications to GORD
- Complications of II, III, IV:
- Upper GI bleeding → iron deficiency anaemia
- Gastric ulcers
- Gastric perforation
- Gastric volvulus
- Total gastric obstruction
- Total gastric obstruction is characterised by Borchadt triad which is severe epigastric pain, unproductive retching and inability to pass a NG tube
- Cameron lesions
