Phone Call/Presentation Questions
- What is the urine output? (How much urine has been passed in the past 24 hours)
- Oliguria = urine output <400mL/day (<20mL/h)
- Anuria ⇒ mechanical obstruction of bladder outlet, blocked IDC or obstructed single kidney
- How are we measuring this and why?
- How much does the patient weigh?
- Does the patient have abdominal pain?
- Generalised abdominal pain ⇒ ? acutely distended bladder with urinary retention
- Is the patient eating and drinking?
- Other observations?
- Does the patient have an indwelling urinary catheter?
- Reason for admission?
- Does the patient have an IVC?
Instructions
- If IDC in place and the patient is anuric ask the nurse to flush the catheter with 20-30mL of normal saline
- Request blood for FBC, UEC and creatinine
- Serum potassium of >5.5mmol/L ⇒ Hyperkalaemia
Prioritisation
- Urgently assess patient with painful urinary retention with urine output <20mL/h or daily urine output of <400mL
- Can be a sign of AKI which can cause hyperkalaemia and fluid overload
- Otherwise can wait for high-priority problems, provided patient is not in pain and serum potassium is not elevated
Common Causes (Corridor thoughts)
- Normal urine output in a healthy individual should be between 0.5-1.5 mL/kg/hour, and patients should generally be urinating at least every 6 hours (Geeky Medics: Measuring & Recording Urine Output).
- Pre-renal
- Absolute decrease in circulating blood volume causing hypoperfusion:
- Inadequate fluid intake e.g. after surgery
- Increased loss of blood or fluids (haemorrhage, burns, erythroderma, hypertheymia, GI fluid losses such as vomiting, diarrhoea, NG suction, renal losses such as diuretics and glycosuria)
- Third spacing of fluid e.g. in pancreatitis, bowel obstruction
- Cardiac failure
- MI (cardiogenic shock), CCF
- Effective decrease in blood volume (vasodilation)
- Sepsis, anaphylaxis, neurogenic Shock
- Vasodilatory drugs, anaesthetic drugs
- Obstruction to circulation
- Constrictive pericarditis, cardiac tamponade, PE
- Locally reduced renal perfusion
- Renal artery or renal vein occlusion (2° thrombosis or stenosis)
- Noradrenaline, adrenaline
- NSAIDs, ACE-i
- Absolute decrease in circulating blood volume causing hypoperfusion:
- Intra-renal
- Acute tubular necrosis
- Usually 2° to pre-renal causes
- Medications (e.g. aminoglycosides, amphotericin B, IV contrast, chemotherapy)
- Poisons (e.g. ethylene glycol, mercury, carbon tetrachloride)
- Endogenous substances (e.g. myoglobin, Bence-Jones protein, amyloid)
- Glomerulonephritis
- Interstitial nephritis
- Pyelonephritis
- Medications (e.g. NSAIDs, penicillins, cephalosporins, sulfonamides, ciprofloxacin, rifampicin)
- Malignancy (e.g. lymphoma or leukaemia)
- Systemic disorder (SLE, sarcoidosis, hypercalcaemia)
- Acute tubular necrosis
- Post-renal
- Upper renal tract obstruction
- Stone, blood clot, sloughed papilla (single kidney)
- Retroperitoneal fibrosis, retroperitoneal tumour
- Lower urinary tract obstruction (bladder outlet obstruction)
- Prostatic hypertrophy, carcinoma of the cervix
- Stone, blood clot, urethral stricture
- Catheter blockage
- Upper renal tract obstruction
WARNING
- A reduced urine output may be the earliest manifestation of shock; restoration of urine output >0.5mL/kg/h signifies restoration of adequate renal perfusion
- Oliguric acute renal failure may be associated with hyperkalaemia, hypertension or acute pulmonary oedema
- Sequelae of acute renal failure include:
- Hyperkalaemia
- Metabolic acidosis
- Acute hypertension (see Hypertension)
- Pulmonary oedema secondary to salt and water retention
Assessment
End of Bed
- How does the patient look?
- A restless patient with abdominal discomfort, agitation and a sensation of needing to pass urine suggests an acutely distended bladder
- Sometimes urinary retention and/or ↓ urine output can have no obvious problems
A → E Assessment
- Heart rate and blood pressure?
- ↑HR by >20 beats/min + ↓SBP by >20mmHg or any ↓DBP ⇒ significant hypovolaemia → pre-renal hypoperfusion
- However ↑HR alone may be due to ↓ intravascular volume, pain of distended bladder or infection
- Acute hypertenstion with oedema may result from acute glomerulonephritis
- Temperature?
- Fever suggests sepsis which could be 2° to UTI, pyelonephritis or systemic bacteraemia
Selective History and Chart Review
- Review patient’s history and hospital course looking for factors that predispose to pre-renal, renal or post-renal causes of decreased urine ouptput with ANKI
- Review observations and fluid balance chart for fluctuations in fluid intake, urine output and body weight
- Medication chart:
- Nephrotoxic drugs, especially in combination such as ACE-i with diuretic and NSAID; aminoglycoside with amphoterecin B; IV contrast material with an ACE-i; or a patient in CCF given an NSAID
- Dose the onset coincide with the commencement of the nephrotoxic drug?
- Potassium supplements worsen hyperkalaemia
- Recent blood urea and creatinine values
- Urea-to-creatinine ratio >20 with specific gravity of >1.020 or urine sodium concentration of <20mmol/L suggests a pre-renal cause
- Urea-to-creatinine ratio <10 with urine specific gravity of <1.020 or urine sodium concentration of >20mmol/L suggests a intrinsic renal cause (e.g. ATN)
Examination
| Examination | Notes |
|---|---|
| Vital signs | Repeat now |
| Note skin temperature and colour | |
| Tachycardia or postural BP changes from dehydration | |
| Hypertension | |
| Mental status | Altered mental status ⇒ cerebral hypoperfusion, uraemic encephalopathy |
| HEENT | Jaundice (hepatorenal syndrome) |
| Scleroderma facies | |
| Dry tongue and mucous membranes ⇒ dehydration | |
| Resp | Basal crepitations, pleural effusions ⇒ CCF |
| Tachypnoea ⇒ CCF or hypoventilation in metabolic acidosis | |
| Pleuritic chest pain ⇒ uraemia, SLE, neoplasm | |
| CVS | Pulse volume |
| ↑ JVP ⇒ CCF | |
| ↓ JVP/flat neck veins ⇒ dehydration | |
| Pericardial friction rub ⇒ uraemia, SLE, neoplasm | |
| GIT | Enlarged kidneys ⇒ hydronephrosis 2° to obstruction, polycystic kidney disease |
| Enlarged bladder ⇒ bladder outlet obstruction, blocked IDC, neurogenic bladder | |
| Rectal | Enlarged prostate gland ⇒ bladder outlet obstruction |
| Pelvic | Cervical or adnexal masses ⇒ ureteric obstruction 2° to cervical, uterine or ovarian cancer |
| Skin | Rash ⇒ acute interstitial nephritis |
Livedo reticularis on lower extremities ⇒ hypoperfusion, embolic renal failure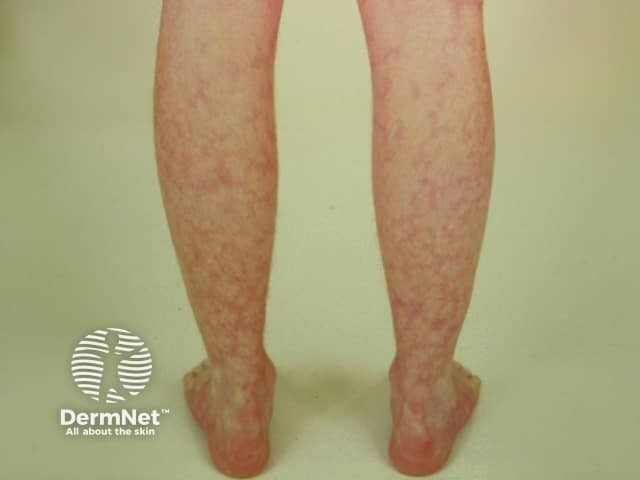 1 1 | |
| Pruritic excoriation ⇒ uraemia, drug rash |
Investigations
- Take bloods for FBC, UEC and blood glucose
- UEC: look for hyperkalaemia
- FBC: Normal Hb suggests acute renal impairment whereas ↓ Hb suggests chronic renal impairment
- LFTs, autoantibodies accordingly as suspected
- VBG for raised anion gap metabolic acidosis from uraemia
- Glomeruloneohritis concern
- Complements C3, C4
- Lupus ANA dsDNA
- Endocarditis multiple blood cultures
- Cryoglobulonaemia usually occurs because of hep C
- PT3 ANCA for ANCA positive vasculitis
- Complements C3, C4
- Perform ECG
- Look for signs of hyperkalaemia: peaked T waves, depressed ST segments, prolonged PR interval, loos of P waves and wide QRS complexes
- Look for evidence of MI or the widespread concave elevation of pericarditis
- Urine dipstick
- If normal CT and no concern for UTI consider a glomerulonephritis to be the underlying cause
- Bedside bladder scan to measure residual bladder volume in obstruction
- Collect urine for dipstick analysis and send to laboratory for MCS including cells and casts, plus urinary electrolyte testing
- Specific gravity
- SG >1.025: highly concentrated urine associated with dehydration and pre-renal failure
- SG 1.010: may be associated with chronic renal disease
- SG <1.005: inability to concentrate urine (ATN, pyelonephritis)
- Haematuria (stone disease, pyelonephritis, GN with >70% dysmorphic RBC)
- Proteinuria (nephrotic syndrome, GN, pyelonephritis, CCF, myeloma)
- Leucocytes and nitrites (UTI, pyelonephritis)
- Urine microscopy
- Leucocytes, Gram-stained organisms, erythrocytes, epithelial cells
- RBC casts are diagnostic of GN
- WBC casts (especially eosinophil casts) are seen in acute interstitial nephritis
- Pigmented granular casts are seen with ATN
- Oval fat bodies are suggestive of nephrotic syndrome
- Specific gravity
Immediate Management
NOTE
Every evaluation for ↓ urine output should begin with ruling out urinary retention
- Nil IDC present:
- Check post void residual volume with a bladder scan and assess for urinary retention
- Insert an IDC to accurately monitor fluid balance
- Lower urinary tract obstruction by insertion of an IDC
- If there has been bladder outlet obstruction, the initial urine volume on catheterisation is usually >400 mL and the patient experiences immediate relief
- After catheterisation for urinary retention, watch for a post-obstructive diuresis by measuring urine volumes hourly
- Lower urinary tract obstruction by insertion of an IDC
- IDC present:
- Ensure IDC is not clogged or kinked
- Flush a blocked IDC with 20-30mL sterile normal saline to resolve intraluminal blockage causing anuria
- Ensure IDC is not clogged or kinked
- If obsstruction is ruled out:
- Assess volume status based on history, clinical situation, JVP and IVC ultrasound (do not give IV fluids to a patient in urinary retention)
- Assess for kidney injury using bloods and urinalysis
- Rule out emerging sepsis
- Attach continuous non-invasive ECG, BP and pulse oximeter monitoring to the patient
Life Threatening Complications
- Severe hyperkalaemia:
- Give 10% calcium chloride 10mL IV over 2-3 minutes to provide immediate cardioprotection to prevent cardiac arrest
- Reduce serum potassium level:
- Give 50mL of 50% dextrose IV with 10 units of soluble insulin over 20 minutes
- Give salbutamol 5-10mg nebulised or 200-500mcg salbutamol IV slowly; repeat doses may be given
- Give 8.4% sodium bicarbonate () 50mL IV over 5 minutes if the patient is acidotic, provided there is no volume overload; works best in combination with dextrose/insulin therapy and salbutamol
- Follow up with potassium exchange resin: calcium resonium 30g PO or enema
- Hypotension with intravascular depletion
- Restore the intravascular volume with normal saline in pre-renal failure; give IV fluid bolus 20mL/kg normal saline repeatedly as needed
- Observe the effect of this fluid challenge on the pulse, JVP, BP and urine output aiming to optimise renal perfusion by reversing hypovolaemia
- Acute pulmonary oedema
- See APO
- In addition to upright, oxygen, gtn, frusemide:
- Give frusemide if pre-renal perfusion is normal
- Consider CPAP and/or IV GTN after consultation with senior doctor
- Monitor diuresis with hourly urine measures and frequent checks of vital signs
- Arrange urgent dialysis if the patient remains volume overloaded, severely acidotic and/or hyperkalaemic
Specific Management
- Identify cause and cease all inappropriate medications (Potassium supplements and potassium-sparing diuretics, NSAIDs, ACE inhibitors)
- Leave a note to inform the usual medical team if on call
- Reduce the dose of renally excreted medications that cannot be stopped immediately (e.g. aminoglycosides)
- Consider indications for dialysis; consult senior and call ICU:
- Hyperkalaemia (>6.5mmol/L) refractory to conventional therapy
- Severe and symptomatic metabolic acidosis (pH <7.1)
- Fluid overload unresponsive to diuretics
- Uraemic encephalopathy with symptoms of decreased mental status, obtundation and seizures or uraemic pericarditis
Other Considerations
- Consider getting the nursing staff to do a two hourly bladder scan