- Comatose = requires painful stimulus to rouse or if GCS ≤8
Summary1
- Check for the patient for a response
- If patient responds
- Call for help if necessary
- A to E assessment
- Examine the pupils (size, equality and reaction to light)
- Measure the blood glucose (if <4.0 mmol/L give 50 mL of 10% glucose solution IV and repeat BGL, repeating dose if necessary)
- Attach monitoring (or pads)
- Obtain IV access and take blood samples for investigation
- Check patient’s drug chart for reversible drug-induced causes of depressed consciousness
- Check allergies
- If patient does not respond
- Call for help
- Turn the patient onto their back
- Open the airway using head tile and chin lift or risk of cervical spine injury use jaw thrust or chin lift in combination with manual in line stabilisation of the head and neck
- If life threatening airway obstruction persists despite effective application of jaw thrust or chin lift, add head tilt a small amount at a time until the airway is open
- Keeping the airway open, listen and feel to determine if the victim is breathing normally. This is a rapid check taking <10 seconds observing for:
- Look for chest movement (breathing or coughing)
- Look for any other movement or signs of life
- Listen at the victim’s mouth for breath sounds
- Feel for air on your cheek
- Assess for carotid pulse
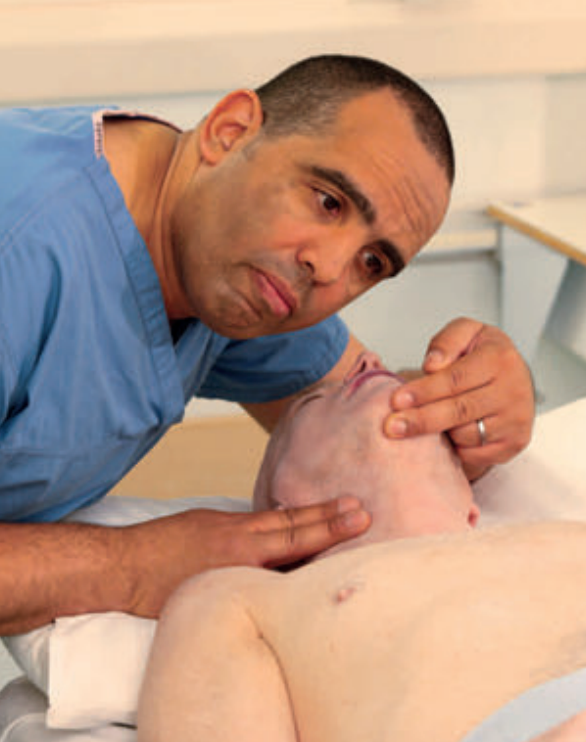
- If signs of life or pulse follow as in step 2
- If patient breathing and has a pulse follow Respiratory arrest
- If no signs of life and no pulse follow ALS and begin CPR
- Review any documentation on the patient (‘alert’ bracelets or wallet cards)
- Review the patient’s notes and other charts
- Nurse unconscious patients in the lateral position if their airway is not preotected
Causes
- Metabolic
- Meds (e.g. opiods, benzos, gabapentin, muscle relaxants, antihistamines)
- Hypo/hyperglycaemia
- Hypercapnoea
- Stimulant withdrawal absuse
- Hypoxia/respiratory failure
- Opioid substance abuse
- Neutrological
- Ischaemic stroke
- Intracranial harmorrhage
- Post-ictal state (⇒ ? underlinyg cause of seizure)
- Non-convulsive status epilepticus
- CNS infection (e.g. meningitis)
- CNS trauma (e.g. epidural or subdural haematoma)
- Other
- Shock/sepsis
- Hypoperfusion
- Hypoactive delirium
- Hyperthermia (e.g. sepsis)
- Hepatic, renal or endocrine failure
Other Notes
- Most common causes
- Poisoning (including alcohol and carbon monoxide)
- Hypoglycaemia
- Post-ictal state
- Stroke
- Head injury
- Subarachnoid haemorrhage
- Respiratory failure
- Hypotension
- Consider in patients who have been abroad:
- Cerebral malaria
- Typhus, yellow fever, trypanosomiasis and typhoid
- Rabies, Japenese B encephalitis
- Severe acute respiratory syndrome (SARS), viral haemorrhagic fever
Assessment
- Initial assessment of ABC and only progress forward once oxygenation and perfusion are stabilised
- Disability (GCS, AVPU, painful stimulus)
- Environment, exposure and extended examination
- Temperature
- Fingerprick glucose
- Focused neurological examination
- Pupillary constriction ⇒ opioid toxicity or brainstem pathology
- Neck stiffness ⇒ meningitis or SAH
- Subtle facial or ocular twitching ⇒ ongoing seizure activity
- Evidence of head or spine trauma → palpate the skull and neck and look in ears for haemotympanum
- Lateralising signs including on fundoscopy
- History
- Cardiovascular risk factors (e.g. HTN, DM, smoking, prior MI) ⇒ iscahemic stroke, intracranial haemorrhage
- New medication, recent ↑ medication dose or AKI (causing decreased renal clearance) ⇒ medication side effect
- Recent head trauma ⇒ intracranial haemorrhage
- Dementia ⇒ hypoactive delirium
- Active infection ⇒ sepsis, delirium
- Drug abuse history ⇒ drug intoxication/withdrawal
- Hx of COPD especially if newly on oxygen ⇒ hypercapnoea
- Hx of diabetes ⇒ hypo/hyperglycaemia
- Exam
- Hypotension, tachycardia ⇒ sepsis, shock
- Focal neurological findings ⇒ ischaemic stroke, recurrence of prior stroke symptoms
- New onset urinary and/or faecal incontinence ⇒ post-ictal state
- Diagnostic
- Fingerprick glucose
- Venous blood gas to rule out hypercapnoea
- Urine toxicology scan
- Neuroimaging if indicated:
- New focal neurological findings
- Recent head trauma or unwitnessed fall
- Anticoagulation
- Suspected seizure
Management
- Call senior
- Stabilise airway, breathing and circulation:
- Supplemental oxygen and pulse oximetry monitoring
- Spinal immobilisation (if possibility of trauma)
- Non-invasive ECG and BP monitoring
- Reliable IV access
- 50 mL of 50% glucose IV (if fingerprick glucose <2.5 mmol/L)
- Administer thiamine 250 mg IV prior to this if the patient is alcoholic or appears malnourished (avoids precipitating Wernicke’s encephalopathy)
- Titrating 200 microgram boluses of naloxone IV every 5 minutes (if evidence of opioid toxiicty)
- Rapid IV fluid resuscitation if in Shock
- Antibiotics if fever and/or neck stiffness
- Commence cooling or warming if temperature abnormal
- Urgent CT scan in unresponsive patient with any evidence of head trauma, lateralising neurological signs or undiagnosed coma
Source
Footnotes
-
As from ALS2 booklet ↩