Type 1: Hypoxaemia with normal (or low) PaCO X 2
Primarily a failure of oxygenation
Usually responds to oxygen therapy
Type 2: Hypoxaemia with an increased PaCO X 2
Failure of ventilation and oxygenation
Requires ventilatory assistance as well as supplemental oxygen
ABG results of PO X 2 CO X 2
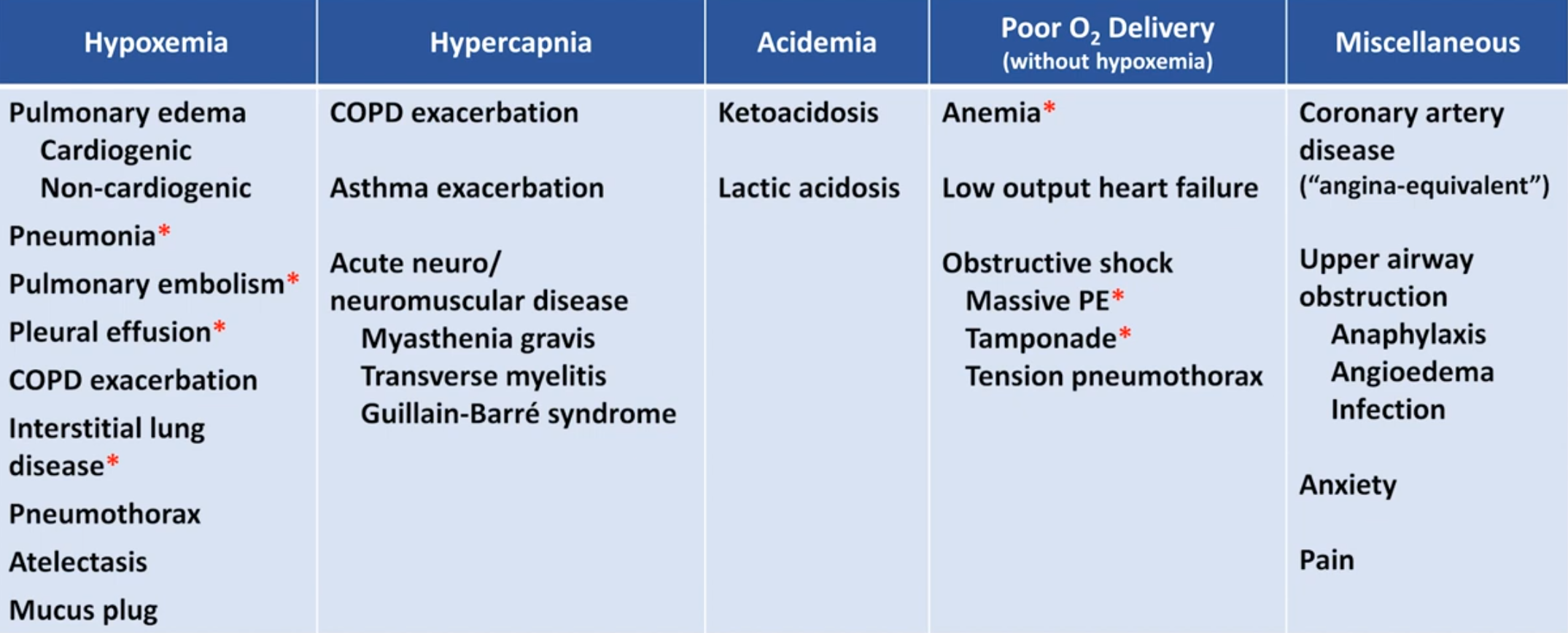
Causes
Acute obstruction Pulmonary
Cardiovascular
Neuromuscular
Depressed level of consciousness
Muscular weakness (Guillain-Barré syndrome, myaesthenia gravis, muscular dystrophy)
Drug intoxication (opioid, sedative)
Poisoning (carbon monoxide, opioid)
Most common aetiologies for acute dyspnoea in hospitalised patients:
Alveolar problem
Flash Pulmonary oedema (e.g. due to tachyarrhythmia, ischaemica/ACS, hypertensive emergency, TACO)
Aspiration pneumonitis
TRALI
Airway problem
Anaphylaxis
Angioedema
Mucous plug
Endotracheal tube dislodgement
Pulmonary embolism
Pneumothorax (post-procedure)
Tamponade (post-procedure, post-MI)
Overview of Assessment and Management
Always call for help
Give oxygen
Assess the patient
CXR/ABG/VBG
Consider adjuncts
Escalation of care
Assessment
Can remember as RATES (respiratory rate, auscultate, trachea position, effort of breathing and saturation)
Airway Patency
Assess airway function
Signs of partial airway obstruction:
Hoarse voice, inability to speak or cough
Stridor, snoring or gurgling secretions
Soft-tissue retraction-tracheal tug, rib or abdominal recession
Loss, or an uncoordinated rise and fall, of the chest and/or abdomen
‘See-saw’ pattern of chest and abdominal movement: the chest is drawn in and the abdomen expands on inspiration and the opposite occurs on expiration
Altered level of consciousness or mental status or agitation
GCS ≤8
Features of partial airway obstruction
Tripod position
Reluctance to speak or cough
Increased work of breathing with nasal flaring accessory muscle use
Inspect
Upper airway for foreign material if possible or using laryngoscopy
Erythema or urticaria with lip, tongue or palatal swelling
Listen for bronchospasm and examine for circulatory features that suggest Anaphylaxis
Localised trauma, burns infection or tumour
Palpate the anterior neck, including the thyroid cartilage for pain, inflammation, crepitus, swelling or masses
Investigate for any cause of depressed consciousness (e.g. hypoglycaemia or opioid intoxication)
Signs and features of complete airway obstruction
No stridor, airway sounds or breath sounds on lung auscultation
Inability to ventilate the patient with a bag-mask
Rapid development of cyanosis and unconsciousness
Link to original
Work of breathing
Signs include: ↑ RR, use of accessory muscles, soft-tissue recession, ↑ HR, sweaty/clammy skin
Effectiveness of respiratory function (saturation probe)
Hypoxia
Cyanosis (oxygen saturation <88%)
Cardiac ischaemia or arrhythmias
Acidosis from tissue hypoxia (lactic acidosis)
Anxiety, agitation or depressed consciousness
↑ A-a gradient on ABG
Hypoventilation
Vasodilation
Headache, drowsiness and lethargy
Asterixis
Acidosis - respiratory acidosis (inadequate removal of CO X 2
Respiratory decompensation
Decompensation is when severe or prolonged respiratory insult causes exhaustion or a reduction in the patient’s physiological reserves
Signs of decompensation
Gasping
↓ respiratory effort
Sweating, lethargy, apathy, drowsiness and coma
Tachycardia → bradycardia (preterminal sign)
Respiratory arrest followed by cardiac arrest
If a patient has any features of decompensation, call senior staff or a MET call immediately
Diagnose the cause
Common conditions which can progress to respiratory failure:
Suggested Diagnosis
By History
Cardiovascular risk factors (e.g. HTN, DM, smoking, prior MI) ⇒ APO
Aspiration risk factors (e.g. post-stroke, sedating medications) ⇒ Aspiration
Intrathoracic pressure within the last 24 hours:
Thoracocentesis, central line, PPM insertion ⇒ Pneumothorax
Pericardiocentesis, PPM lead extraction ⇒ tamponade
New medication started recently
Anphylaxis (<6 hrs)
Angiodema (days)
Transfusion within last 6 hours ⇒ TACO, TRALI
By Exam Finding
Hypotension ⇒ PE , ACS , Pneumothorax , tamponade, Anaphylaxis
Bilateral crackles ⇒ APO , Aspiration
Wheezing ⇒ Non-specific
Asymmetric lung findings ⇒ Aspiration, Pneumothorax , mucous plug, ET tube dislodgement
Signs of DVT ⇒ PE
Investigations
Investigations to consider and typical prioritisation in acute respiratory distress
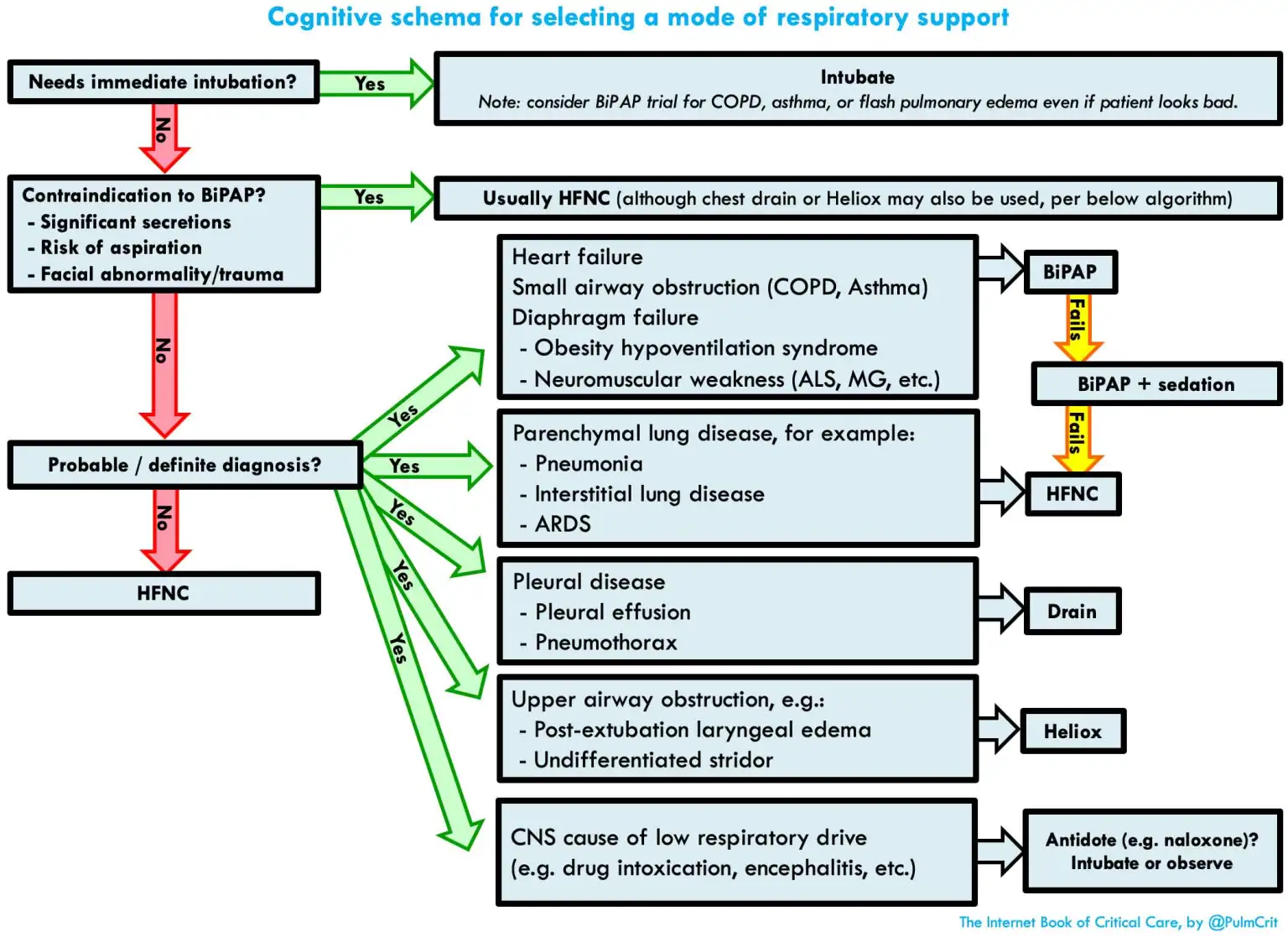
Management
Sit patient upright
Do not neglect airway issues and place heavy importance of suctioning if relevant (e.g. aspiration, mucous plugging)
Use supplemental oxygen in all hypoxic patients with high-flow oxygen at 15 L/min through a mask with a reservoir, (target oxygen saturation > 90-92%)
High inspired oxygen concentrations do not depress ventilation in patients who are in respiratory distress
In patients with COPD who chronically retain CO X 2
Giving too much oxygen to patients who chronically retain CO X 2 CO X 2
Changes in pulmonary vasoconstriction, dead space and shunting (V/Q mistmatch)
Haldane effect (haemoglobin molecules release CO X 2
Blunting of the hypoxic drive; these patients depend on mild hypoxia to stimulate their respiratory centre
If unsure if they are a chronic retainer, check any previous blood gas results
Begin empirical O X 2
Increase/decrease oxygen delivery until O X 2
Recheck blood gases and watch for a change in P CO X 2
Continue with current therapy if CO X 2
Decrease oxygen deliver if CO X 2 O X 2
If CO X 2 see ventilation below
Blood gases are necessary to determine the adequacy of ventilation (can use either venous or arterial as it will likely not influence immediate management) - see ABG Interpretation
If wheezing, consider bronchodilators (see: COPD Exacerbation ) perhaps nebulised
Rule out tachy-arrythmia or demand related ischaemia if you can prior
If signs of APO consider nitrates if BP tolerates
Avoid jumping to diuretics in a euvolaemic patient with pulmonary oedema
Consider reversing opiates
Consider NIV
Ventilation
Ensure the patient has not received respiratory depressants (e.g. opioids) in the past 24 hours (e.g. check pupils)
Give naloxone 0.2mg up to 2mg IV, SC or IM every 5 minutes repeated until alert
Be careful to avoid a withdrawal reaction: Start at 100 mcg IV in opiate-dependent patients
Bag valve mask assisted manual ventilation may be required in a patient with ↓ LOC until definitive ventilation is available
Consider: CPAP, BiPAP ventilation or NIV machines
If still no improvement contact ICU and make arrangements for ETT intubation
Acute respiratory acidosis with a pH <7.2 usually requires mechanical ventilation until the precipitating cause can be reversed
Disclaimer: These notes are for educational purposes only and are not medical advice. I do not claim copyright for the content or images unless otherwise stated. For concerns or changes, create a new issue on GitHub .
Created with Quartz v4.5.2 © 2026